INTRODUCTION
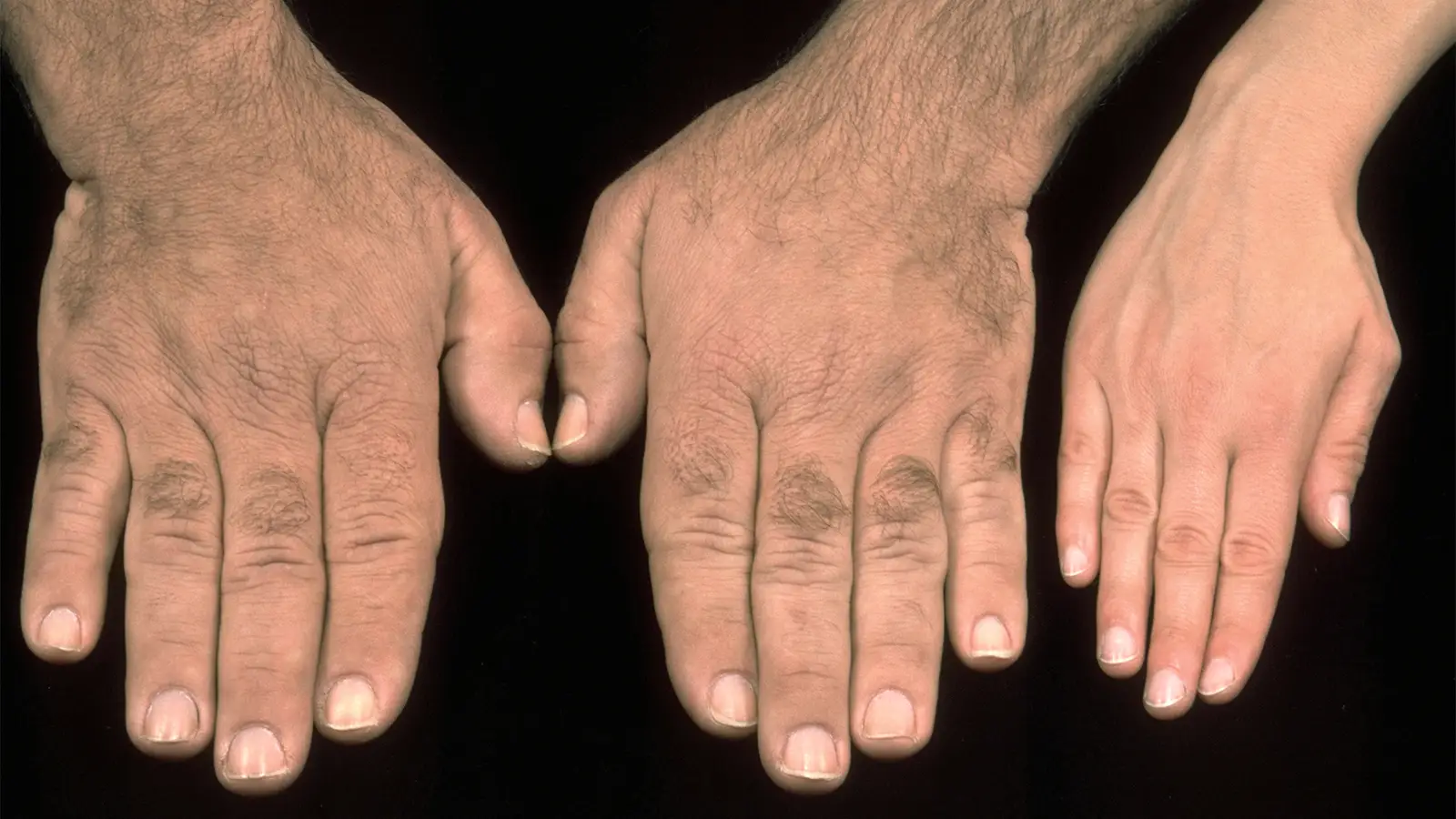
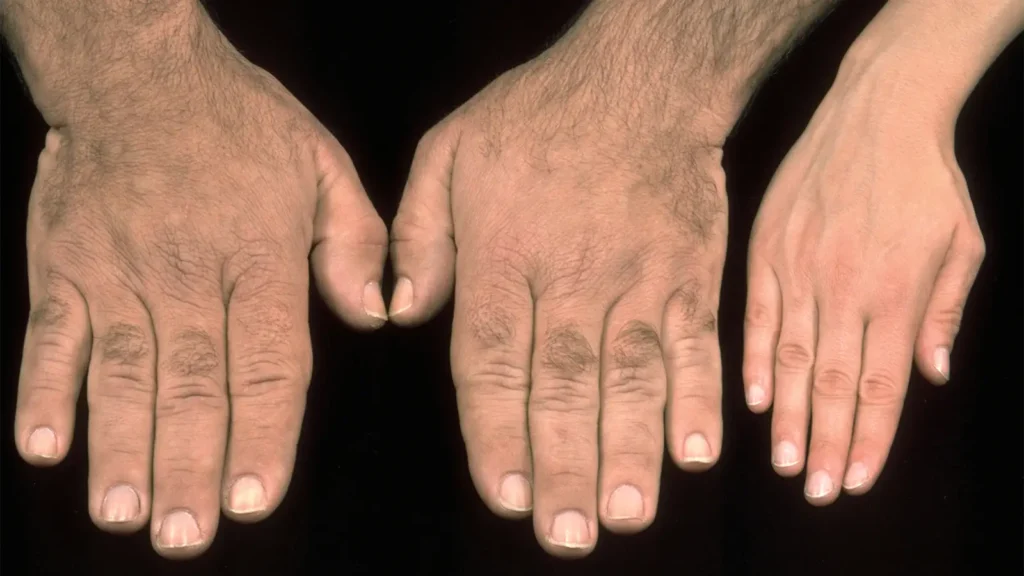
Acromegaly is almost always caused by a somatotroph (growth hormone [GH]-secreting) adenoma of the pituitary gland and is associated with increased morbidity and mortality. As a result, almost all patients should be treated, even those who are asymptomatic and those in whom the disorder does not seem to be progressing. One exception is a patient with a short life expectancy who is not expected to live long enough to benefit from therapy.
The treatment of acromegaly will be reviewed here. The clinical manifestations and diagnosis of acromegaly are discussed separately.
Medical therapy — Several medications are available for treating acromegaly, including some that inhibit GH secretion and one that inhibits its action. Pharmacologic treatment is used when surgery alone has not reduced serum GH and IGF-1 to normal.
Patients for whom a medication can be considered as primary therapy include those who have unacceptable surgical risk, refuse surgery, or have adenomas that are unlikely to be cured surgically.
Somatostatin analogs — Octreotide and lanreotide are analogs of somatostatin (GH-inhibitory hormone) that inhibit GH secretion more effectively than native somatostatin because of their greater potency and longer plasma half-life (two hours versus two minutes). Somatostatin analogs inhibit GH secretion by binding to specific receptors for somatostatin and its analogs. Their effect is greater when the number of receptors is high; repetitive administration does not result in desensitization or loss of therapeutic efficacy.
Octreotide and lanreotide — Octreotide and lanreotide also cause pituitary adenoma shrinkage in some patients. The mechanism of the shrinkage remains unclear. In a study of tissue samples from 32 surgically resected somatotroph macroadenomas, the mean growth fraction of adenomas exposed to octreotide was 83 percent less than those not exposed. However, in another report, octreotide exhibited an antiproliferative effect but no effect on the apoptotic index.
Dose and administration — Two somatostatin analogs, octreotide and lanreotide, are widely available. The long-acting form of octreotide is given as an intramuscular injection once a month. The initial dose is 20 mg once a month. If the serum IGF-1 concentration does not decrease to normal within two months, the dose can be increased to 30 mg and then to 40 mg a month.
Efficacy — Efficacy should be judged by normalization of the serum GH and IGF-1 concentrations, which should eventually be followed by regression of the soft tissue manifestations of acromegaly and by shrinkage of adenoma size. The two once-monthly preparations, octreotide long-acting release (LAR) and lanreotide (autogel or depot) appear to be equivalent for control of biochemical markers and symptoms.
● Predictors of response – Tumor subtypes may be a predictor of response to somatostatin analog therapy. The densely granulated tumors are typically smaller and more active (produce more GH) and respond well to somatostatin analogs. In contrast, the sparsely granulated subtype tumors tend to be larger, more common in females and in younger patients, more invasive, and are relatively less responsive to somatostatin analogs.
● Biochemical improvement – Normalization of serum IGF-1 concentration with somatostatin analogs occurs in 40 to 75 percent of patients. The success rate varies markedly with study design, ranging in two reports from 38 percent in patients who were not preselected for responsiveness to a mean of 66 percent in a review of several studies, most of which included patients who had been preselected for responsiveness to the short-acting form. Combined therapy with cabergoline and a somatostatin analog may be effective when either alone is not.
● Improvement in symptoms – A somewhat greater percentage of patients appear to experience improvement in symptoms with somatostatin analogs than exhibit IGF-1 normalization, presumably because even a partial decrease in GH results in some degree of symptomatic improvement.
Successful therapy is associated with an improvement in several signs and symptoms during the year following a decrease in biochemical parameters:
- Soft-tissue swelling, carpal tunnel syndrome, and snoring
- Sleep apnea
- Left ventricular mass and left ventricular function
- Adenoma size – Somatostatin analog therapy leads to a reduction in adenoma size of approximately 20 to 50 percent in 30 percent of patients. In a 2005 systematic review of patients with acromegaly receiving a somatostatin analog as primary medical therapy (before or as an alternative to surgery and radiotherapy), approximately 37 percent experienced a significant reduction in adenoma size (mean 19 percent). In a subsequent study of 99 patients who received somatostatin analogs as primary therapy, 45 percent had normalization of serum IGF-1 concentration, and 44 percent had a >50 percent reduction of adenoma size.
- Side effects — Somatostatin analogs are usually well tolerated. Approximately one-third of patients have nausea, abdominal discomfort, bloating, loose stools, and fat malabsorption during the first several weeks of therapy, after which the symptoms usually subside spontaneously with continued use.
Somatostatin analogs are associated with an increased risk of gallstone disease. Up to 56 percent of patients develop asymptomatic cholesterol gallstones or sludge during the first 18 months of therapy. However, we do not suggest routine abdominal ultrasound monitoring. We suggest ultrasound only if the patient develops signs and symptoms suggestive of gallstone disease. Less common side effects include hair loss, constipation, and bradycardia.
Octreotide and lanreotide transiently inhibit insulin secretion, but their clinical impact on glucose homeostasis is minimal. This was illustrated by a meta-analysis of 18 trials in patients receiving these analogs for acromegaly. Fasting insulin concentrations were significantly reduced and glucose levels were slightly higher on an OGTT, but there were no significant changes in fasting glucose or glycated hemoglobin (A1C) values.
Pasireotide — The somatostatin analog pasireotide is also effective in some patients with acromegaly and is approved for its treatment, but it frequently causes or worsens hyperglycemia.
Oral octreotide — An oral formulation of octreotide (delayed-release capsules) based on a transient permeability enhancer that enables bioactive gastrointestinal absorption has been approved for use for the management of acromegaly.
Pegvisomant — Pegvisomant is a GH receptor antagonist that is a mutated GH molecule to which polymers have been attached at several sites to prolong its half-life. The mutation results in increased affinity to site 1 on the GH receptor but decreased binding to site 2. As a result, pegvisomant blocks native GH from binding but does not activate the intracellular signaling that mediates its action.
Dopamine agonists — Dopamine agonists, especially cabergoline, may inhibit GH secretion in some patients with acromegaly but do not work as well as somatostatin analogs.